I can still remember exactly how I felt the first time I ever saw my younger sister Anne-Marie “in action.” It was the day after our Dad’s wedding in May 2018. We were delivering the leftover flowers to the residents at the Grove Nursing home in our hometown of Arnprior ON, where she worked during the summer as an RPN while attending Nipissing University.
I won’t lie – my first reaction was mild shock, bordering on disbelief. Don’t get me wrong, I had zero doubts about Anne-Marie’s ability to do her job. She’s smarter and more motivated than anyone I know, myself included. It was seeing the way she interacted with the residents that had my heart unexpectedly swelling with pride.

I was used to the goofy, sarcastic and often aloof version of my sister that we all know and love. Seeing her in a professional setting for the first time gave me a glimpse of another side of her – a gentle, patient and nurturing professional who clearly cared about each and every one of her patients. I listened, pretty much trying not to cry, as my baby sister chatted with each resident, remembering details about each of their families and putting their flowers in water if they asked for it. Even though she wasn’t on the clock, she made sure each resident was comfortable and didn’t need anything before we moved onto the next room. I often joke that I’ll never understand how Anne-Marie can do what she does day in and day out, but seeing how passionate she was that day, I knew that she had found her calling.
Now, here we are exactly two years later and Anne-Marie, who is turning 23 this summer, is now a qualified Registered Nurse (RN). She became registered on March 6, is graduating from Nipissing in June and began her new career at the Georgian Bay General Hospital (GBGH) in Midland a few weeks ago.

Meanwhile, COVID-19 has the entire world gripped in its icy claws, and there seems to be no end in sight. Talk about crazy timing, am I right? I can’t imagine what it would be like to begin such a challenging career as a fledgling nurse in the midst of a global pandemic. So, naturally, I had to get all the gritty details.
“We have been close to or at full capacity since I started in April,” Anne-Marie says. “But on the other hand, I’m glad that I’m not in a hospital that is in a COVID crisis right now. I feel kind of guilty saying that.”
The hospital Anne-Marie works at has had three positive cases of COVID-19. Simcoe County, where GBGH is located, had 360 positive cases in total as of May 8. Every day, Anne-Marie and the other nurses use nasopharyngeal swabs to test dozens of patients per day for COVID-19. Since elective surgeries have been put on hold, GBGH is also converting its Post-Anesthesia Care Unit to a COVID ICU to meet the anticipated demand.
“The hospital has been split into two parts: hot and cold zones,” she says. “Hot is where we send COVID-positive patients.”
Anne-Marie’s floor has been designated a cold zone. However, she says there is still a considerable risk of coming into contact with the virus just by going into work every day. But when I asked Anne-Marie if she was worried about getting sick, she said it wasn’t herself she was worried about.
“I think if I get it I will be fine,” she says. “I am more scared of who I could give it to before I have symptoms, like my other patients who are older and vulnerable. [My boyfriend]’s grandparents also live up the road; his grandpa comes over every day to work the farm and Justin does their grocery shopping for them. So even though we maintain a distance as much as possible, I’m still scared they could get it and they are in their 70’s.”
Anne-Marie says she considers herself lucky that the virus didn’t overwhelm smaller hospitals like GBGH as much as she anticipated it would, but that could change in the coming weeks. As the weather warms up, seasonal cottagers from Toronto are beginning to descend on the area despite advisories from Ontario officials that discourage unnecessary travel to cottages. This could potentially put a significant strain on local resources and access to PPE for the healthcare workers who need them.
Battening Down the Hatches
Anne-Marie believes that beginning her career during the COVID-19 pandemic, in some ways, is similar to how it would have been under more normal circumstances.
“Other than protocols that change every other day and having to wear a mask for 12 hours,” she says. “I hate having to wear the damn mask. I swear I have a little CO2 poisoning by the end of my shift. But then I think of people who have to wear the N95’s and are all gowned up for 12 hours straight and I realize it could be worse.”
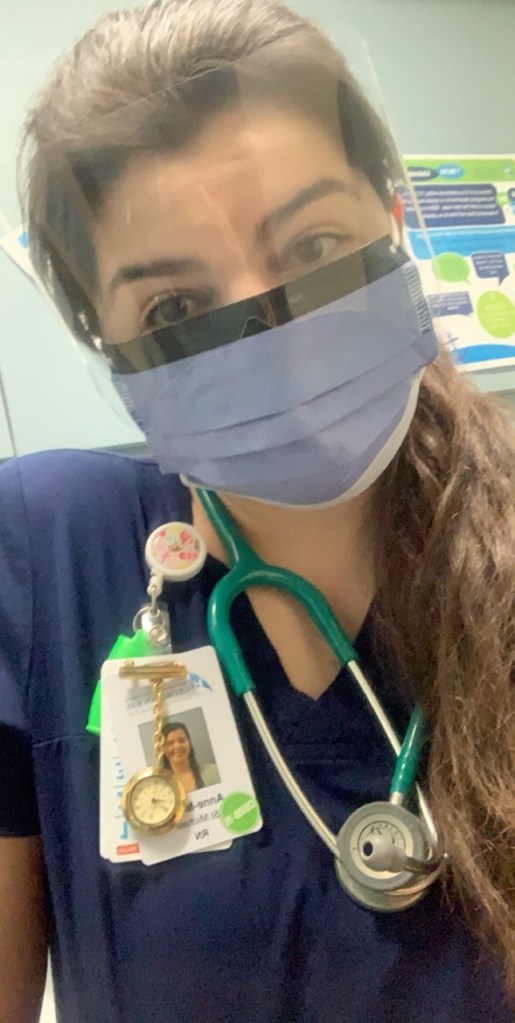
The hospital has taken some drastic precautions to keep both their staff and patients safe. When staff arrive at work, they are given a fresh pair of scrubs that have been washed onsite to change into. At the end of a shift, they leave the scrubs there and change back into their street clothes before leaving to avoid bringing anything onto the floor or back home with them.
All PPE used by staff during a shift must be counted and reported daily. Frontline staff must wear masks with face shields. Patients must also wear a mask when they are outside their room. Anyone going in or out of the hospital is asked the COVID-19 screening questions. Patients moving between floors must be swabbed for COVID-19, and senior patients returning to Long Term Care facilities or group homes must test negative before leaving the hospital.
“Anyone with any of the COVID symptoms gets sent to a hot zone until deemed negative,” Anne-Marie says. “If they get admitted with something other than COVID and they develop respiratory symptoms we swab them and send them to a hot zone until they are negative. We don’t allow any visitors unless the person is palliative. Then it’s one visitor at a time.”
Anne-Marie says the hospital has also implemented a new protocol for Code Blues, which is a medical emergency or cardiac arrest. The new protocol, called Protected Code Blue, requires a lot more training, a lot more PPE and a lot fewer staff, which can make attending a code difficult.
“I think everyone is scared of a code blue now,” she says. “With all the extra PPE and the limited amount of people, it takes much longer to implement and is much harder to do. Compressions don’t seem like a lot of work, but after two minutes you’re sweating and there’s no one to swap out with you.”
Strange Days for Staff and Patients Alike
These safety protocols (although absolutely necessary) can seriously slow things down, making an already long day feel even longer. Especially during your second back to back 12-hour overnight shift at the tail end of a 65 hour work week. However, Anne-Marie says that on the good days, it’s easy to remember that the long hours are worth it. Her shifts begin at either 7 a.m. or 7 p.m., and she says she tries to arrive 10 to 15 minutes early so the previous shift can actually go home on time.
“The unfortunate part is I don’t wake up early enough to drink my coffee, so I drink half before my shift on the drive in and half when it’s cold on breakfast break,” Anne-Marie says. “Its rough.”
Working in these challenging conditions is hard on staff, but Anne-Marie says it’s hard on patients, as well.
“With the masks, it sucks for people with dementia or people who are hard of hearing,” she says. “They are either scared and get more disagreeable if they have dementia or they can’t read lips like they usually do and it’s almost impossible to have a conversation. Plus, without visitors our patients are definitely more lonely. I try to spend a little more time with them, but obviously that’s hard to do.”
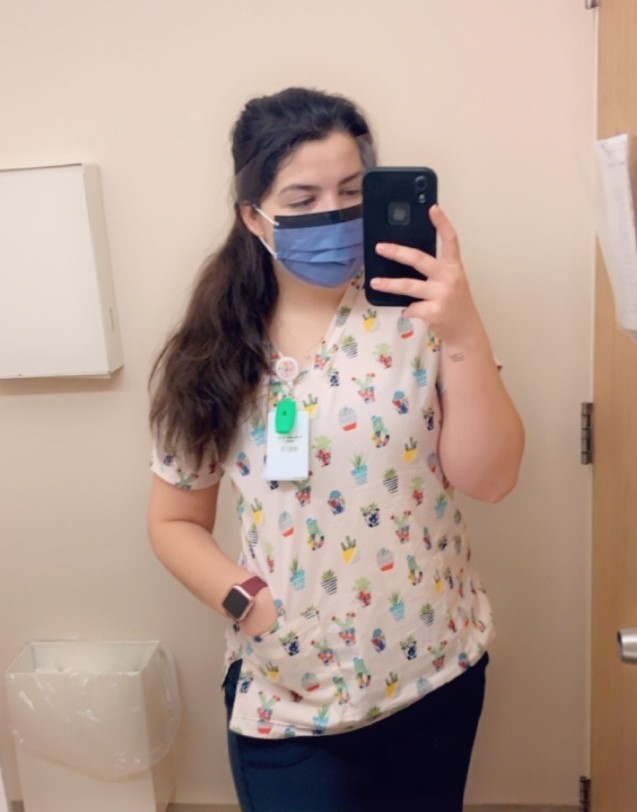
These days Anne-Marie looks after up to seven patients per shift, which doesn’t give her as much time as she would like to spend one-on-one time with each one.
Despite her busy schedule, Anne-Marie says she tries to spend individual time with her patients whenever she can. Some patients, she says, don’t mind being left alone or spend a lot of time on the phone with their families. She says she can usually tell when someone needs to talk, and more often than not is happy to oblige.
“I try to keep it even, maybe around 2 hours per patient, per day,” she says. “I will check in throughout the day and if they feel like talking I’ll stop and take some time to talk to them until I get pulled away for something else. Sometimes palliative patients need a little more time than others. I feel the worst for them right now.”
A Day in the Life
If I’m being honest, my sister does more in a single shift than I probably do in an entire week. After getting the reports from the previous shift, a nurse will typically begin their day with a visual check on their patients and review their charts to check any new orders or appointments in order to organize their day. After that, each patient must have their vitals checked, plus a quick head to toe assessment and their morning medications. On a good day, Anne-Marie says this part alone takes around an hour or an hour and a half.
“Sometimes patients have morning appointments, or diagnostic imaging will call and say they are ready for the patient, or they will have a morning surgery they need to be prepped for so that can put you behind,” she says.
“Then I try to have one or two people washed up and changed before break. After break, I finish getting the rest of my patients washed and comfortable. Check and see if there is any new orders. Send patients down to diagnostic imaging. Do any wound dressing changes or anything like that. Some people have more frequent vitals. Sometimes we will get admissions. Sometimes patients need to be fed so we will have to do that too. Basically after the morning assessment we just make sure our patients are comfortable for the morning.”
At this point, I’m having a hard time coming to grips with the fact that we’re still in the “morning” stage.

After the morning assessment and lunch meds, Anne-Marie says they just “roll with the punches,” doing vitals and assessments as needed, talking to the doctors about patients and carrying out their orders, bringing patients down to diagnostic imaging and other appointments, and most of all hoping that “code blue” doesn’t come over the loudspeaker.
As I sit here writing this story, I can feel myself getting emotional yet again. There’s something that just seems to hit differently about interviewing someone you’re already close with and learning about a different side of their life. I feel fortunate and humbled to have received this insight into the life of a frontline healthcare professional. Most of all, I’m beyond proud that that person is my little sister.
A Brief Rant and Words of Wisdom
At the same time, I find myself becoming frustrated. How can so many of us sit here behind our computer screens, shouting “thank you frontline workers” and adding #NursesWeek2020 frames to our profile pictures, all while protesting against the safety measures being implemented and pushing to reopen the province prematurely? And for what, a haircut?
If you truly support nurses and want to celebrate Nurses Week, the best thing you could do would be to stay home, wash your damn hands, follow the advice of healthcare experts and continuing to practice physical distancing. We aren’t out of the woods yet. The last thing we should be doing is making it more difficult for healthcare workers to do their jobs.
Nurses, just know that there are people who do genuinely stand behind you. We will all get through this together, by each doing our part. I’ll wrap things up with some valuable advice from Anne-Marie, for nurses and other frontline workers who might be feeling the strain right now:

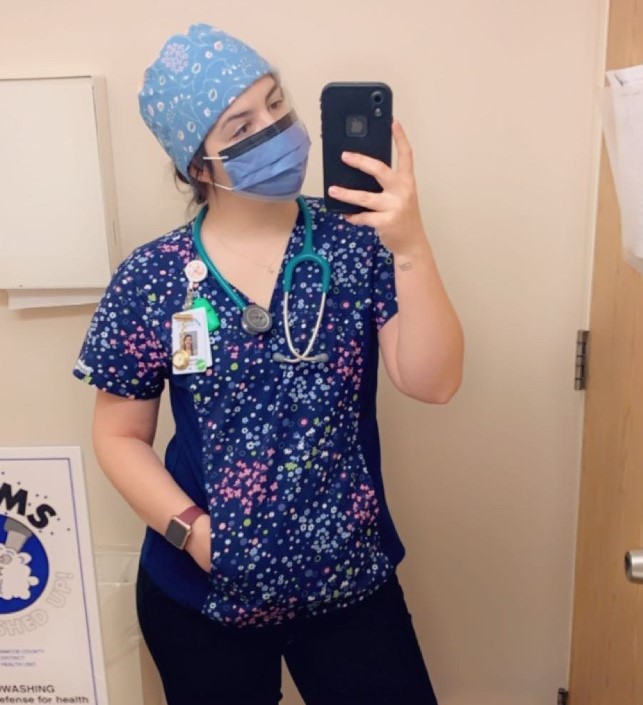
“Make sure to take care of yourself. I know people may feel obligated to help out as much as they can in a crisis. But your body needs rest and nutrition to stay healthy,” she says. “It’s funny that I say that because I’m negative and always burnt out – whoops – but its important for people to listen to their bodies and their limits and take a day off if they need it. If you get sick, you can’t be any help to anyone else.”
Very well written and a great insight to how difficult it must be for front line staff and their patients.
LikeLike