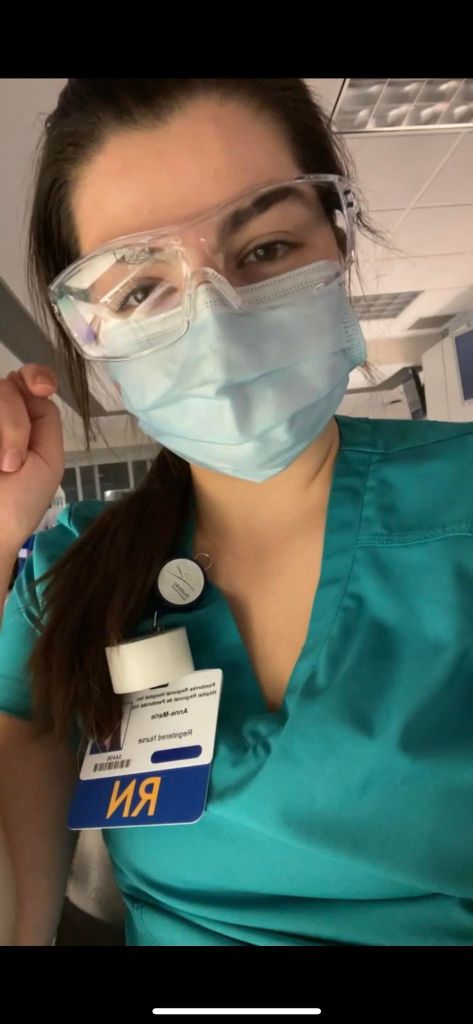
Back in May 2020 I interviewed my younger sister, Anne-Marie, a newly licensed Registered Nurse (RN) launching her career in the early days of the COVID-19 pandemic.
At that time, COVID was brand new. New information was coming out about the virus every day, thanks to global efforts to “flatten the curve.” It was just as new to healthcare workers and scientists as it was to the public, and most experts were learning right alongside us. Anne-Marie was fresh out of school, learning to adjust to her fledgling career at the Georgian Bay General Hospital (GBGH) in Midland, ON.
Now we’re two years into this thing and, frankly, there’s no real end in sight. As COVID-19 continues to mutate into new strains, each growing more and more dangerous in their own ways, sometimes it feels like things are just as uncertain as they were back in 2020.
But some things have changed, and not necessarily for the better.
Here we are, having entered yet another new year trapped beneath the heel of this pandemic, and there is a growing divisiveness that hangs like poison in the air. Conspiracy theories and misinformation seem to be more contagious these days than the virus itself. Our healthcare system is buckling under the strain it continues to endure, and to make matters worse, there has been a significant shift in the way our healthcare heroes are being treated by both government and the public.
People aren’t standing out on their front steps every night banging pots and pans for frontline workers anymore, or delivering donuts, coffee and words of encouragement to their local hospitals. Instead, many are growing tired of the ongoing restrictions and some groups have even taken to protesting outside hospitals. Federal and provincial financial supports for nurses and other healthcare workers have also dwindled across Canada. But we’ll get into that a little later.
Catching Up: Two Years to Flatten the Curve
As for Anne-Marie, it has been an eventful two years. If you’ll permit me a few moments for a big sister brag: not only did she get engaged, but she and her fiancé also recently purchased their first home in Cobden.
She worked the medical/surgical floor at GBGH for eight months, then switched to Labour and Delivery, where she worked for 10 months. After buying her house, she moved back to the Ottawa Valley where she began working full-time in the ICU at Pembroke Regional Hospital. As well, she works on a casual basis in Long-Term Care at the Grove Nursing Home in Arnprior, and in the Labour and Delivery unit at Almonte General Hospital. She is also called in fairly often to help out in the ER.
“To sum it up, I would say nursing has gotten more difficult,” Anne-Marie says. “My abilities as a nurse have improved, but the politics of health care continue to worsen.”
Like many nurses these days, Anne-Marie is feeling burnt out, overworked and undervalued. Hospitals in Ontario are facing an unprecedented staff shortage, especially after many healthcare workers (including nurses) were suspended from their jobs due to strict vaccination mandates. This has left those who remain to pick up the slack.
“I know these staffing shortages are everywhere. I’ve seen it first hand when moving hospitals, where both are suffering,” she says. “We are trying to care for more patients and sicker patients with less staff. There are a lot of new nurses with limited experience working in different specialties in the hospital with limited experienced nurses to help guide them. Nurses are being forced to be redistributed to different areas they may not be comfortable with or trained in.”

A typical work day for Anne-Marie might look something like this: The workday starts at 7 a.m. In the ICU she will typically have one to three patients, depending on the severity of their condition and how many patients are admitted at that time. ICU nurses must follow strict standards of care, including a head to toe assessment of each patient every four hours at minimum. If their condition warrants it, these assessments can happen as often as every 15 minutes; this can get complicated when she has three patients to look after. Aside from that, her ICU duties are fairly similar to what they would be on the med/surg floor.
“We assess the patients, give them their medications, help them get washed up, and do whatever wound dressing changes or other interventions they need,” she says. “In LTC, I either do meds and dress changes or I’m the charge nurse and go around doing paperwork and putting out fires all day.”
On Labour and Delivery, nurses are responsible for caring for their patients from labour to postpartum. “There’s not really a routine there,” she says. “If there’s someone in labour then we’re supporting them. If it’s postpartum it’s a lot of education and supporting with infant care and breastfeeding. Doing assessments on mom and baby.”

Each shift lasts 12 hours. Anne-Marie typically works up to 48 hours per week at her full-time job, not counting any extra shifts she might pick up. She works days and nights on a six-week rotation of two days two nights, and then three to six days off before another set. That also doesn’t count her casual work, or all the overtime she has taken on to help out with staffing shortages. Needless to say, this doesn’t leave much room on her schedule for wedding planning.
“We have to wear an N95 and face shield at all times now. Your face gets very sore after a 12-hour day,” she admits. “We have to wash our face shields between each patient. Nurses are frequently having to care for more patients than is safe to do so. It’s hard knowing you’re not providing the best care possible to your patients because you only have enough time to give each patient the bare minimum.”
Canadian Healthcare Crumbling Under Pressure
At the time of our last interview, most hospitals had a designated COVID floor. This meant that although nurses and other healthcare workers were still at risk, their exposure to the virus was limited. Today, the number of COVID-positive patients has overwhelmed the units. There are now COVID patients on every floor, which makes it more difficult to mitigate transmission to staff and other patients. This has led to more stringent precautions, not only for staff, but for patients and visitors as well.

“Every patient is swabbed for COVID and put on extra precautions until they test negative,” Anne-Marie says. “Even then, if they have COVID symptoms they might not be cleared from infection control. So then each patient interaction also requires an isolation gown and gloves.”
This may not seem like a big deal, but she says it takes a nurse valuable time they don’t necessarily have to get all dressed up in the required PPE, just to bring a patient a glass of water.
“Visitors have to be fully vaccinated,” she continues. “I feel like the visitor policy changes every day. Right now, COVID-positive patients are not allowed visitors. COVID-negative patients can have one primary caregiver able to visit.”
Canada’s nursing staff shortage predates the pandemic. Between 2018 and 2019, the Canadian Nurses Association reported a 1.5 per cent decline in employed nurses. However, COVID-19 has exacerbated things to a point where those who remain are so burnt out, many are opting to change careers entirely.
“One girl from Arnprior is leaving to be a hair dresser,” Anne-Marie says. Another nurse in New Brunswick abandoned her 12-year nursing career at 42 years old to become a long-haul trucker.
Let me give you a better picture of how things stand today. According to the Canadian Institute for Health Information, in 2020 Ontario had the lowest nurse-per-capita ratio in Canada. At the time there were 665 RNs for every 100,000 people, putting us well below the Canadian average of 814. This means Ontario would need 22,003 more working RNs just to reach the national average. Though I was unable to find statistics for 2021, healthcare workers with boots on the ground say these numbers have only grown more dire in the intervening months.
To name one example, a hospital in Orangeville has redeployed kitchen/dietary staff to work with nurses on inpatient floors… a move of clear desperation, considering these employees are not even certified to work in healthcare.
Anne-Marie says that while she believes healthcare workers should be responsible for coming to work fully inoculated against COVID-19 (just like they are required to be up to date on any other vaccination, she adds) she is also torn by the sheer desperation of the current situation. She says Ontario hospitals could use all the able-bodied nurses they can get right now. Asking doctors and nurses to risk working alongside unprotected coworkers on a daily basis is dangerous, but so is expecting them to contend with 100+ hour work weeks, inadequate staff coverage and dwindling resources, not to mention their own rapidly deteriorating mental health.
“Older, seasoned, and knowledgeable nurses are leaving the profession,” Anne-Marie says. “This is really unfortunate because they are great leaders and mentors for us newer nurses.”
Bill 124: Nurses in a Stranglehold

Another source of frustration among the nursing community in particular is Bill 124, or the Protecting a Sustainable Public Sector for Future Generations Act, which received Royal Assent and was passed in November 2019 by the Ontario Government.
Essentially, the controversial Bill caps compensation for nurses in contract negotiations for pay increase to one per cent every three years. This prevents nurses from bargaining for increased pay, more sick days and much-needed mental health supports. While the average RN salary can be anywhere from $57 to $71 thousand per year, according to a December 2021 letter to the provincial government by the Registered Nurses Association of Ontario, the salary cap imposed by Bill 124 falls well below Ontario’s inflation rate.
In practice, this actually translates to a significant annual pay cut.
“I don’t have any nice words to say about Bill 124,” Anne-Marie says. “People may think nurses are being selfish since we make a decent living and are demanding a higher raise. What most people don’t know is that other male dominated professions, such as police and firefighters, are exempt from the Bill.”
“During this pandemic, nurses are risking their health and their sanity,” she continues. “We are being told they can change our schedule, they can order us to come in for mandatory overtime, they can deny our vacation, they can relocate us wherever they deem fit, they can give us unsafe patient ratios. Nurses are being stripped of their rights and then further disrespected by this Bill.”

While nurses were included in the federal government’s $3 billion wage boost for essential frontline workers early on in the pandemic, they have had little financial support since then. Not only does this make it glaringly obvious how performative the supportive words from the Ontario government have been, but it makes nurses feel undervalued. Disposable. Fed up.
“Nurses are tired and done with it,” Anne-Marie says. “Doug Ford is disrespecting nurses and it’s embarrassing. He can open all the hospital beds he wants, but without nurses those beds are useless.”
The Ontario government has also reportedly asked nurses to volunteer their time to work at vaccination clinics, while paying physicians more than $100 per hour to do the same job. Some physicians are paid more than $200 per hour for this work, according to the Ontario Nurses Association. Opposing political forces, including Ontario Green Party Leader Mike Schreiner, have criticized Ford’s administration for not affording nurses the same basic respect as physicians for doing the same work.
“Doctors and medical students are also being asked to perform nursing duties under the supervision and guidance of RNs for a pay rate of $170 to $220 per hour,” says Anne-Marie. This is not only a massive insult financially, but it also asks nurses to devote additional time and effort (which they don’t often have) to oversee the work being done by these doctors and med students.
“Yet somehow, paying physicians four times more to be supervised by nurses makes more sense than giving us a raise,” she adds.
Life in the Misinformation Age

The COVID-19 pandemic sets itself apart from pandemics of days past in a myriad of ways, but perhaps the most stark difference is the number of people who have decided, en masse, to actively go against the recommendations of Public Health officials and other experts in the field.
Of course, there have always been dissenters. For example, 1955 saw the first wave of mass vaccinations of North American children against polio. Prior to the development of the polio vaccine, this debilitating disease was simply a terrifying fact of life. When the vaccine was finally approved for public use, much like today, there was a chunk of the population who were vehemently against its use. Others, much like today, cited the vaccine as a government manipulation tool for social control. Ultimately, though, the polio vaccination campaign was successful. According to NPR, this was because back in 1955, there was a widespread trust in medical experts, media and yes, the government, that simply does not exist today.
This is purely speculation on my part, but I truly believe social media and the Internet have a lot to do with why that is. Today, our level of access to information is unprecedented. At any given moment, we have an unfathomable wealth of information at our fingertips–or rather, in our pockets. Anyone can go online and essentially say whatever they want, with full confidence that they know exactly what they’re talking about.
The role of the mainstream media has shifted–journalists no longer decide what information is and is not fit for public consumption. Instead, the role of a journalist is now to wade through the endless sea of information and filter it as best as possible, hoping against hope that the public will take it seriously. Unfortunately, however, trust in journalism has largely fallen to the wayside, much like it has for doctors, scientists and other experts in the medical field.
I’m an outspoken advocate for both freedom of expression and the incredible access to information provided by digital media. However, refusing to acknowledge its role in creating and perpetuating the “misinformation epidemic” would be naïve.

It only takes a quick, 30-second scroll through your social media feed to see that misinformation abounds, especially in online spaces where COVID deniers, conspiracy theorists and anti-vaxxers can congregate easily, with massive reach. This type of rhetoric can be the catalyst for someone who may have legitimate hesitancies about the vaccines turning to more extreme viewpoints.
In journalism, we have an unwritten rule of thumb: if it can’t be confirmed by at least two additional (reputable) sources, it’s not fit to claim as fact. Unfortunately, the general public doesn’t have to abide by this rule before clicking “post.” Few people bother to fact-check themselves, or even check if the information they’re consuming and sharing is actually true. There are some of us who will share an article on social media without even reading it first or checking whether the source is legitimate, which Anne-Marie says often times, it isn’t.
“People don’t know where to find reputable data and believe everything they read on Facebook or on a quick Google search. Unfortunately, that information tends to be incorrect,” Anne-Marie says, “and the spread of false information has a direct impact on the healthcare system. The more misinformation that’s out there, the less people there are that get vaccinated. Unvaccinated people are more likely to be admitted to hospital which means they’re taking up beds with a preventable disease.”
Myth Busting
Speaking of misinformation, one of the biggest rumours circulating the online sphere right now is that the vaccine doesn’t actually prevent the spread of COVID-19. So what’s the point in “making people get it” if it doesn’t work?
“No vaccination is 100% effective,” Anne-Marie reminds us. “The vaccine is to protect people from severe illness or death and protect those around you. Those who are vaccinated are less likely to contract COVID, less likely to spread COVID, less likely to require hospitalization, and are contagious for a shorter period of time. Vaccination helps prevent hospitalization.”
While experts have confirmed that COVID-19 vaccines do not always prevent the transmission of COVID-19 between patients, especially newer variants like Omicron and Delta, being vaccinated can make a world of difference when it comes to symptom severity, especially in immunocompromised patients.
Anne-Marie adds that this is important because Canadian hospitals are already facing a bed crisis, excluding COVID admissions. “There are many sick people with chronic conditions that require hospitalization,” she says. “Then you have the acute issues like surgeries and traumas that require beds. If our hospitals are filled with COVID patients, we don’t have room for the unpreventable admissions. Most people with the vaccine who get COVID are able to recover safely at home.”
Not only are unvaccinated people admitted to hospital more frequently than those who are up to date on their inoculations, but Anne-Marie says those who are unvaccinated end up with greater oxygen requirements, adding to the burden and strain placed on hospital resources and staff.

“Social media also lets people who don’t understand science or statistics share information,” Anne-Marie points out. “For example, people are saying that less unvaccinated people have contracted COVID than vaccinated. More than 80 per cent of our population in Ontario is vaccinated, which means that the statistics will already be skewed. But people don’t think about that.”
Similarly, contrary to what the memes will tell you, Anne-Marie says the number of vaccinated individuals admitted to the ICU does not actually exceed the number of unvaccinated patients. “We COVID swab every admission to the hospital now,” she says. “We have had many vaccinated people be admitted to the hospital with other issues and end up being COVID-positive with no symptoms. These people count towards the COVID admissions in hospital, but they are being treated for other conditions.
“Of all the COVID-positive people we have had in the ICU, only the unvaccinated people were admitted for management of COVID. I have had multiple vaccinated asymptomatic COVID patients who were 70 plus. I have also had unvaccinated patients who were young and required intubation.”
The Experts Are Only Human
One often-cited reason for the growing mistrust in doctors, scientists and other healthcare experts is how much the information and recommendations have changed, and continue to change over time.

“I definitely understand the frustration with the ever-changing rules,” Anne-Marie says. “It feels like every day there are new government restrictions and new policies being released in the hospital. However, I think we have to be patient as new research and information comes to light. No one has experienced a pandemic on this scale, so no one knows the best way to manage it.”
And that’s the thing that, I think, a lot of people seem to have forgotten: the people in charge are human beings. Human beings who make mistakes and adjust based on learning new information. Like I mentioned, they have been learning about this virus right alongside the rest of us. That’s how science works: as we learn more about the virus itself and its impact, information is bound to change.
Yes, sometimes that new information contradicts something that was originally stated. But that does not erase the credibility of the doctors, scientists and officials who have dedicated their entire lives to the study of immunology and healthcare. And it certainly doesn’t mean Uncle Greg, who barely graduated high school and “does his own research” exclusively on 4chan and Reddit forums, right-wing tabloids and his own Facebook timeline knows better than the experts do.
“Do I always agree with all the ever-changing rules and back and forth? No, I don’t,” Anne-Marie says. “But at the end of the day we can only work with the information we have available to us. People need to understand that the restrictions aren’t just put in place to control people. They’re there to help reduce the burden on the healthcare system.
“Hospitals are already struggling with no more beds, and not enough nurses to staff the ones we do have. If we have a surge of sick COVID patients requiring hospitalization, we’re not going to have anywhere to put them.”
Performative Support: “A Slap to the Face”
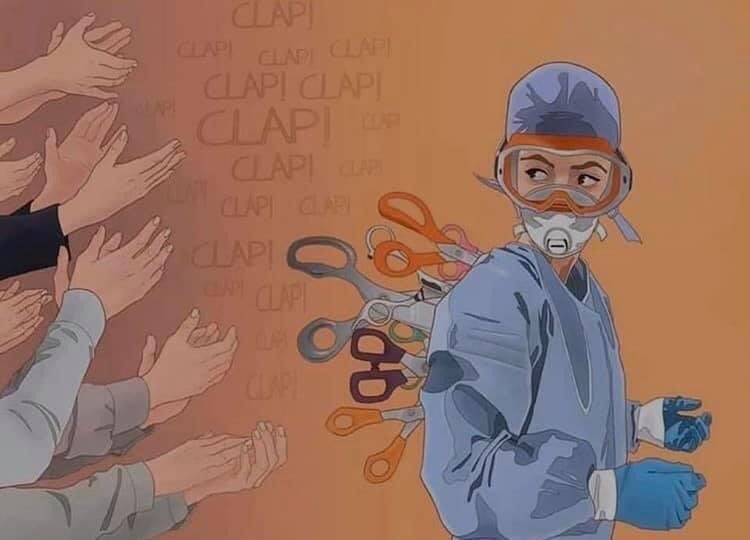
Anne-Marie says that while she does believe most people respect the nursing profession, now more than ever, some members of the public (and even government officials) have shifted to a more negative attitude.
“People understand how difficult it must be to be on the front lines during this pandemic,” she says. “However, I feel as though most people don’t outright disrespect nurses, but their actions do. When people disregard wearing a mask, getting the vaccine, or other recommended health measures, it feels like a slap to the face.”
She adds that nurses have been vocal about the struggles they are currently facing. By not following guidelines, Anne-Marie says people are sending the message that they really don’t care that nurses are drowning right now. She says these people either don’t understand what’s going on behind the scenes within hospitals, or they don’t care.
“You don’t care about the health of the people around you, let alone yourself,” She adds. “When you say COVID isn’t real, or COVID isn’t that serious, it’s discrediting the hard work that healthcare workers have been doing since the beginning of this pandemic.”
“I was reading a post on how nurses feel since the beginning of the pandemic, and a member of the public wrote in saying that nurses should have known there was a risk for a pandemic when signing up for the job, so we can’t complain. And that she lost respect for the profession who clearly only cares about the money. I was like, wow. I wonder how many people think like this?”
In terms of the provincial government, Anne-Marie says as much as they claim to respect healthcare workers and as grateful as they claim to be for their hard work, again, their actions say otherwise. Many of the Ford administration’s actions, including the decision to reopen schools and forego the reporting of outbreaks and COVID cases within classrooms, has placed unnecessary strain on the frontline healthcare workers they claim to be so dedicated in supporting.
“Short staffing, no pay compensation, and denying vacation doesn’t exactly show respect or gratitude to the profession that is bearing a large burden of this pandemic,” Anne-Marie says.
Mental Health a Rising Concern for Patients & Staff Alike

Since she has started taking on shifts in the ER, one other alarming thing Anne-Marie has noticed has been the uptick in patients experiencing mental health emergencies.
“There has been a significant increase in mental health presentations to the Emergency Department lately,” she says. “From young teenagers to the elderly. On multiple days, there have been four or more people in ED with mental health complaints within a 12 hour shift.”
She continues that COVID has exacerbated feelings of stress, anxiety, and isolation. The frequent lockdowns and endless, ever-evolving restrictions have caused a variety of issues for Ontarians. These include the closing of schools, loss of income, isolation from others, and loss of social supports. “This mental health crisis is just as debilitating as the bed crisis we are currently facing,” she warns. “Mental health supports were lacking prior to the pandemic. Our province is not able to keep up with this trend.”
But it’s not only the patients who have experienced increased mental health-related symptoms in the two years since the onset of the pandemic… the hospital staff are feeling it, too. A February 2021 survey of 18,000 Canadian healthcare workers by Statistics Canada shows seven in 10 healthcare workers reported worsening mental health as a result of COVID-19. Nurses in particular struggled with declining mental health, with 37 per cent reporting poor mental health compared to only 27 per cent of doctors.

Anne-Marie pointed me to an interesting U.S. study by the Kaiser Family Foundation, which suggests that the fallout of COVID-19 on rates of mental illness and substance abuse will continue to present itself well past the “end” of COVID’s reign of terror. The study recommends that governments and public health agencies begin putting the necessary supports in place now, to avoid a large-scale crisis in the very near future.
Whether that will actually happen remains to be seen.
I asked Anne-Marie if she had any advice for her fellow healthcare workers when it comes to managing their mental health. “I’m probably not the best to give advice on how to avoid burnout and stress,” she says, laughing. “The main thing is to remember that it’s not your individual responsibility to fix a broken system. Do not risk your physical and mental health to staff a hospital that would replace you in a heartbeat. You can’t pour from an empty cup.”
Challenges & Triumphs
Don’t worry, folks. Anne-Marie has assured me that she has no immediate plans to ditch nursing and become a bull-rider or something. Her first two years as an RN have been full of challenges, but she says they mostly concerned the politics surrounding nursing, rather than the job itself.
“Between Bill 124 and the staffing crisis, it’s a difficult time to be a nurse,” she admits. “Many people are leaving the profession, leaving the rest of us to pick up the pieces. I don’t blame people for leaving. It’s a difficult job, and it’s even worse when you feel that you aren’t respected for the physically, mentally and emotionally draining work you do each day. Nurses see things on a daily basis that people wouldn’t imagine seeing in their lifetime and then have to carry on with their day like nothing happened.
“Nurses are one of the only professions that deal with verbal and physical abuse with no consequences to the abuser. I’ve been hit, kicked, bitten, punched, scratched, and screamed at on many occasions. It is also difficult when we’re short staffed and I don’t have time to do my best. I know the days when I feel like I have neglected a certain patient because they were medically stable and I needed to give more attention to someone else who was sicker. 12 hours seems like a long day, but now nurses are having nine patients to care for; it’s impossible to provide good care.”
But even now, she says the good that comes with nursing makes the bad days worth it.
“The most fulfilling part is always the same, knowing that I have made a positive difference, when I have time to go above and beyond to care for a patient,” Anne-Marie says. “Sometimes it’s as simple as a conversation, but it makes a difference. Being able to support and provide comfort to people during scary, vulnerable times is an honour. Those moments of gratitude from a patient and their family are what keeps me going during these hard times.”
In Conclusion (I know, finally)
As for me, I couldn’t be more proud of my brilliant, talented, hardworking, hilarious and goofy baby sister.
The only thing I have left to say is this: to some of you, COVID may seem like no big deal. It may seem like just a glorified flu, or an annoyance that’s keeping you from getting your nails done or going out to eat with your friends. To some of you, the restrictions may seem silly and unnecessary. To some of you, the uncertainty you feel toward the vaccine may outweigh your responsibility to do your part in protecting your community.

But some of us have family and loved ones working in healthcare. We have sisters, brothers, mothers, fathers, aunts, uncles and friends who face the terrifying realities of this pandemic every single day. These are people we care about more than anything in the world.
So if not for yourself, do it for them. Care. Act. Do it for the people who continue to put themselves at risk for you, even when you spit in their face. Do it for the people you claim to support. We’re all tired, we’re all frustrated.
Do your part in helping to finally end this damn thing.
© Victoria St. Michael 2022



Wow, very welll written Victoria, enjoyed reading about my niece Anne Marie the nurse, and knowing my niece Victoria is such an awesome reporter!! Cindy St. Michael-Bennett
LikeLiked by 1 person
Thanks for reading, Auntie! Anne-Marie is a total badass, I’m so proud of her. Love you!
LikeLike
The reach of conspiracy theories and misinformation, which is now being weaponised by the far right, is deeply disturbing. Something we may be stuck dealing with for decades to come, unfortunately.
Anyone in healthcare seem to be at a higher risk of burn out as the majority of them are seriously over worked and underpaid
LikeLiked by 1 person
Absolutely, you hit the nail on the head. Thanks for your comment!
LikeLike